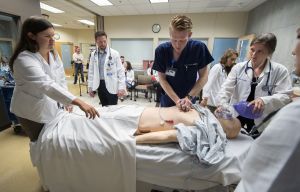
Credit: Steve Zylius/UCI
A landmark study has found that simulations are just as effective as a teaching tool, if not better, than clinical rotations.
When preparing healthcare students for a career in patient care, simulation is becoming a vital teaching tool for clinical training.
That’s more true than ever as instruction goes online.
Assistant clinical professor and nurse practitioner Tiffany Nielsen is the simulation coordinator at the UCI Sue & Bill Gross School of Nursing.
Her goal from day one has been to grow the program and provide students with innovative experiences that make them better nurses.
Equivalent, if not better than clinical rotations
The California Board of Registered Nurses (BRN) recommends that up to 25% of clinical time can be replaced with simulation. The percent has been temporarily raised to 50% to accommodate students during the coronavirus pandemic.
A landmark study by the National Council of State Boards of Nursing (NCSBN) validated simulation as an effective training tool in lieu of direct patient care, leading to the development of national simulation guidelines for prelicensure nursing programs.
“It can be just as good, if not better, than clinical rotations,” Nielsen says.
Mistakes in simulations won’t injure or kill patients, while instructors can guide and direct student learning more intently.
Instructors can also create specific situations and patient conditions for students to experience, something that can’t be done in the hospital.
Simulation resources required
A simulation program requires ample resources, Nielsen says. Just implementing a single simulation scenario takes significant time, manpower, and supplies.
It all starts with a high-tech, talking manikin with a heart beat, pulses and lung sounds. The manikin blinks and its pupils respond to light. Students can perform various procedures, including administering medications and inserting IVs and foley catheters.

Credit: Steve Zylius/ UCI
During the activity, the students are observed through one-way glass while a specialist operates the high-fidelity manikin.
Each simulation is based on a scenario determined by the faculty subject matter expert and specific course learning objectives, for example, responding to a coding patient.
Nielsen works with the faculty to ensure that the goals of every simulation are met.
During the activity, the students are observed through one-way glass while a specialist operates the high-fidelity manikin.
“We provide them with the scenario and instructions on exactly what to do and how to evolve the scenario,” she says. For example, the operation specialist may increase the manikin’s heart rate in response to pain or a medication the students administer during the simulation.
The specialist is also the voice of the manikin, which can respond as the students ask questions and interact with the simulated patient.
Standardized patients are also frequently used in scenarios to play the role of nervous parents or concerned loved ones. Nursing students are evaluated on how well they communicate, educate and interact with them.
Debriefing after a scenario
While the simulation is critical, the debrief is even more important.
When the scenario is complete, the faculty and students go into a debriefing room away from the manikin and simulation room.
“We break down what happened, what went well, what didn’t go well, and so on,” Nielsen says.
Students are asked to explain why they chose a particular course of action and offer their rationale and insights. Nielsen says their actions may have been correct, but the reasoning behind them misguided or unintentional.
“Debriefing is where the majority of learning actually takes place,” she says.
It’s crucial that facilitators are trained on debriefing techniques, so students can be guided to reflect upon and dissect their actions and learn from them.
Online learning during a pandemic
Now that instruction has transitioned to online learning due to California’s stay-at-home orders, simulations have been running a little differently. But they are no less high-tech: Students and faculty are now using virtual patients and simulation platforms to provide students with patient care experiences from a distance.
“At first, I was worried,” Nielsen says of how students and faculty might do with the shift and new technology. “But from the feedback I have received thus far, it’s very positive.”
Users can interact with the virtual patients to:
- Collect a health history
- Check vital signs
- Look up lab and imaging reports
- Review the electronic health record and provider orders
- Perform a physical assessment
From there, they create a plan of care, prioritize and execute nursing interventions, and assess the patient’s response.
Nielsen says the programs then offer the students feedback on what was done well and what was missed or delayed.
Faculty also receive a report, where they can see how long each student spent in a scenario, the actions they took, and what topics require further review.
Expanding simulations in the future
Nielsen says simulation has been incorporated into almost every prelicensure nursing course, and more are coming.
Eventually, the nursing school will have its own building that includes a simulation lab. Currently, they share space with other programs.
When the state-of-the-art simulation lab opens, it will be a powerful tool in the education of future nurses. It will also be open to nurses and other professionals throughout the community and state who want to advance their skills and reach higher levels of expertise.
“Interdisciplinary teams is the direction healthcare is going,” she says. “As part of the College of Health Sciences, we are transforming education to reflect that collaboration and simulation is a crucial component.”
